 
In a value-based care model, length of stay and 30-day readmissions impact provider reimbursements. Insurance providers, or payors, assess the medical codes to determine how they will reimburse a provider for their services. 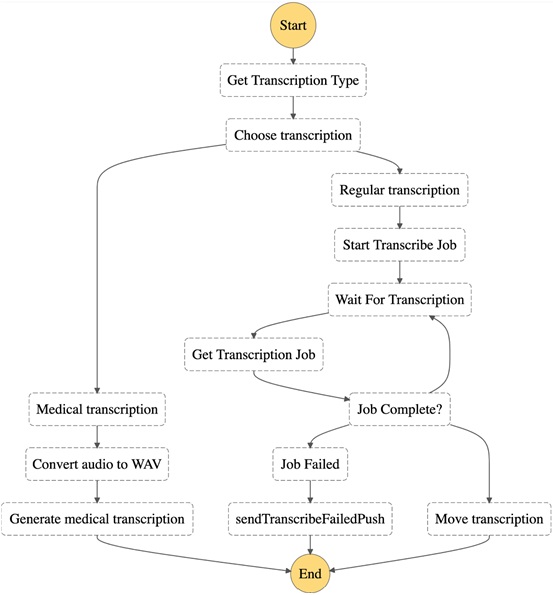
When a provider submits a claim, they include all relevant medical codes and the charges for that visit. The medical codes describe any service that a provider used to render care, including: This bill contains unique medical codes detailing the care administered during a patient visit. 
What is a medical claim?Ī medical claim is a bill that healthcare providers submit to a patient’s insurance provider. In this blog, we’ll help you learn the basics about medical claims: what they are, where they come from and what they mean. It can be difficult to do all this without fully understanding medical claims data. Healthcare organizations can use this claims information to: All-payor claims contain detailed diagnosis and procedure information for any billable patient visit. Interested in learning more? Fill out the form and one of our representatives will get back to you to answer all your questions.Medical claims are some of the most valuable sources of data for healthcare organizations. But that’s only because trained and profession Medical Billers and Coders do their jobs!Īt YTI Career Institute, you can train to become a Medical Billing & Coding professional at our Lancaster campus in as little as 12 months. If you’ve ever had a medical procedure, you know costs can add up and you’re probably thankful that insurance companies cover most of those costs. Those codes that will become second nature to you make certain insurance companies have accurate information and patients receive the benefits they’re entitled to. The whole reason you’ll learn about medical codes is to bill insurance companies properly.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
